Cancer
Our articles and data visualizations rely on work from many different people and organizations. When citing this entry, please also cite the underlying data sources. This entry can be cited as:
Max Roser and Hannah Ritchie (2018) - "Cancer". Published online at OurWorldInData.org. Retrieved from: 'https://ourworldindata.org/cancer' [Online Resource]
Max Roser and Hannah Ritchie (2018) - "Cancer". Published online at OurWorldInData.org. Retrieved from: 'https://ourworldindata.org/cancer' [Online Resource]
This article was first published in July 2015; last revised with substantial revision in March 2018.
Every sixth death in the world is due to cancer, making it the second leading cause of death (second only to cardiovascular diseases).1 In 2016, 8.9 million people are estimated to have died from the various forms of cancer. The Institute for Health Metrics and Evaluation (IHME) put relatively small error margins around this global figure: the lower and upper estimates extend from 8.75 to 9.1 million.2
Progress against many other causes of deaths and demographic drivers of increasing population size, life expectancy and — particularly in higher-income countries — aging populations mean that the total number of cancer deaths continues to increase. This is a very personal topic to many: nearly everyone knows or has lost someone dear to them from this collection of diseases.
Cancers are defined by the National Cancer Institute (NCI) as a collection of diseases in which abnormal cells can divide and spread to nearby tissue. As this definition suggests, cancers can arise in many parts of the body (leading to a range of cancer types, as shown below) and in some cases spread to other parts of the body through the blood and lymph systems.
I. Empirical View
I.1 Global perspective on cancer prevalence
What is the prevalence of cancers across the world's population? The charts below provide data on the share of a given population with any form of cancer. This is first shown collectively across all cancer types, followed by breakdown by cancer type. Overall, we tend to see a higher prevalence of cancers in higher-income countries - strongly attributed to the increased risk of cancer from particular lifestyle factors such as smoking, diet and obesity, and alcohol intake. Prevalence of cancer ranges from approximately 2 percent of the population, down to around 0.2 percent.
When broken down by cancer type we see that globally breast cancer is the most prevalent form, followed by colon & rectum, and prostate cancer. Across most countries these are the top three cancer forms, however they tend to vary in their ranking across the world.



Number of people with cancer
How many people in the world have cancer? Globally, it's estimated that 42 million people across the world suffered from any of the forms of cancer. This number has more than doubled since 1990 when an estimated 19 million had cancer. The chart below shows the total number of people with cancer across all countries of the world.
Also shown in the charts below is the breakdown of cancer numbers by type. As we explored above, the prevalence of breast cancer is highest globally; an estimated 8 million had breast cancer in 2016; 6.3 million had colon & rectum; 5.7 million with prostate; and over 2.8 million with tracheal, bronchus & lung cancer.


I.2 Cancer prevalence by age
The visualisations below detail the breakdown of cancer prevalence by age, as well as the age-specific prevalence rates across populations. Overall, we see that globally the majority of cancers occur in those aged 50 and over. Approximately 83-84 percent of known cancer cases occur in those aged over 50, with 46 percent aged 50-69 and 37 percent aged over 70 years old.
Just over one percent of global cancers occurs in children and adolescents aged 14 years and under. These cases are predominantly childhood cancers within the group of leukaemia.


I.3 Global perspective on cancer deaths
Whilst we largely focus on the global pattern of cancer deaths, all of the data presented here – based on estimates from the IHME's Global Burden of Disease programme – is available to explore by country using the "change country" function at the bottom of the interactive charts which follow.
In the chart below we see the total number of deaths in 2016 attributed to the range of cancer types. With more than double the number of attributed deaths of the next leading form, 'tracheal, bronchus, and lung cancer' claimed the largest number of lives at more than 1.7 million in one year. Next follow 'stomach cancer', 'colon and rectum cancer', and 'liver cancer', all with a similar number of deaths, at around 830,000 globally in 2016.
This chart also allows exploring deaths by country (click 'change country' at the bottom of the chart).
In exploring patterns across various countries, we see that 'tracheal, bronchus, and lung cancer' is the leading form of cancer deaths across most high and middle-income countries. However, the leading form in lower income countries varies: colon and rectum; liver; cervical; stomach; breast and prostrate all top the list in several countries.

If we look at how the number of cancer deaths has changed since 1990 — as in the chart below — we see that global deaths have increased from around 5.7 million to 8.9 million over this period. Note you can scroll over this chart to see the annual number of deaths by type over time. For clarity, we have grouped all cancer types with less than 100,000 global deaths in 2016 into a collective category 'Other cancers'.
If we switch the chart below to "relative" mode we can compare how the distribution and share of deaths across the various cancer types has changed since 1990. With just under 20 percent of the total, 'tracheal, bronchus and lung cancer' have the highest share at the global level. Overall, we see that the relative share of deaths across cancer types has remained largely stable with time. Some notable changes occurred in stomach cancer (which has fallen from 13.8 to 9.4 percent); esophageal cancer (falling from 5.7 to 4.7 percent); liver cancer (rising from 8.2 to 9.3 percent); and pancreatic cancer (rising from 3.6 to 4.6 percent).

I.4 Cancer deaths by age
How are cancer deaths distributed across age groups?
In the chart below we see the breakdown of total cancer deaths by broad age category, ranging from under-5s to those over 70 years old. Overall, we see that the majority of cancer deaths occur in those over 50 years old; 44 percent of cancer deaths in people aged 70+ years old, closely followed by 43 percent aged between 50 and 69. The distribution of deaths across the age spectrum has changed notably since 1990; the share of deaths which occur in those aged over 70 has increased by 7 percent, whilst the share in those aged 50-69 and 15-49 has fallen by approximately 3-4 percent each.
Collectively, children and adolescents under 14 years old account for less than one percent of cancer deaths — although still tragically, this equates to around 80,000 children per year.

I.5 Are death rates from cancer rising?
With an increase in global cancer deaths from 5.7 to 8.9 million since 1990 (an increase of 56 percent), and similar trends in the number of absolute deaths across most countries, it may seem reasonable to assume that cancer death rates are on the rise. But is this really the case?
Whilst a crucial metric of total disease burden and mortality, the absolute number of deaths has two key caveats: it fails to account for changes in population size and age structure. As we have explored above, the majority of cancer deaths occur in those aged over 50 years old; this means we should expect the total number of cancer deaths to increase as a population ages. The drivers of rising life expectancy, aging populations, and population growth can compound to give a skewed perception of frequency.
A more useful metric in this regard is the age-standardized death rate. This metric corrects for the effects of changing age distributions by normalising to a fixed reference population structure (assumed the same across countries and with time), and for differences in population size by reporting as the number of deaths per 100,000 individuals.3 The age-standardized death rate from all cancer types are shown in the visualisation below. This data can be explored through time using the 'play' button at the bottom of the chart, and national time-series can be viewed by clicking on a respective country.
In 2016, we see that most countries have death rates of 50 to 150 deaths per 100,000 individuals. On average, higher-income countries tend to fall towards the upper band of this range; across North America, Europe, and Australasia, rates are typically close to 150 per 100,000. This is also true across a number of countries in Sub-Saharan Africa. Rates across Latin America, Asia, and some parts of Africa are on average lower (50-125 per 100,000).

The number of cancer deaths can therefore be influenced by three key factors: an actual change in the prevalence of cancer, changes in population size, and changes in population age (since we see higher cancer death rates in older individuals within a given population). In the chart below we show an index of three variables since 1990: the total number of cancer deaths (this does not correct for population size or age); all ages death rate (which corrects for population size); and age-standardized death rate (which corrects for population size and aging). These trends are indexed to the year 1990, where all values in 1990 are equal to 100 (a value of 120, for example, would indicate a 20 percent increase since 1990; 60 would indicate a 40 percent reduction).
At a global level we see that total cancer deaths have increased more than 50 percent since 1990. However, when we correct for population size (all ages death rate), this increase is much smaller at just over 10 percent. Finally, once corrected for age, we see rates have actually fallen by 15-20 percent since 1990. In other words, the individual incidence of cancer deaths has actually fallen. These indexed trends are available to view by country in the chart below using the "Change country" option.
The overall global trend nonetheless shows an often counter-intuitive finding: despite increasing numbers of cancer deaths, individual death rates are falling. In 1990, 161 people out of every 100,000 globally died from cancer — by 2016 this had fallen to 134 per 100,000.

For the purposes of assessing the total incidence of cancer, in the chart above we grouped all cancer types together to look at overall trends. However, death rates and progress in reducing mortality incidence varies across the many forms of cancer. In the chart below we see the individual age-standardized death rates across cancer types. This is again measured as the number of deaths per 100,000 individuals.
As we would expect from the leading cause of cancer deaths, rates in tracheal, bronchus and lung cancer are highest globally at 26 per 100,000. This has fallen slightly from approximately 29 per 100,000 in 1990, with even greater declines in some countries (in the US, rates have fallen from 53 to 41 per 100,000).
In some cases we have seen dramatic declines over the last few decades. The most notable is stomach cancer, for which death rates have fallen by more than 40 percent from 22 to 13 per 100,000. Rates in esophageal and cervical cancer have also both dropped by around one-third since 1990.

I.6 Understanding the global cancer disease burden
The overall global trends on cancer mortality — as summarised in data above — tells a story which at first glance can seem conflicting.
The total number of deaths from cancer is increasing. This is predominantly a result of aging (and growing) populations. Once we correct the number of deaths for population size, we see that cancer death rates have approximately flatlined; then when further corrected for age we see that globally, death rates are falling. This represents progress, although very slow.
Death rates have the limitation of being unable to account for the burden of disease from illness or disability - they therefore capture only mortality, and not morbidity. Another metric used to measure disease burden is Disability-Adjusted Life Years (DALYs) lost. DALYs are used to measure total burden of disease - both from years of life lost and years lived with a disability. One DALY equals one lost year of healthy life.
The chart below shows age-standardized rates of DALYs lost from cancers, measured per 100,000 individuals. This is measured across all cancer types. Also shown are disease burden rates broken down by cancer types. We see that at a global level, the largest burden results from tracheal, bronchus and lung cancer, followed by stomach, liver, colon & rectum, and breast cancer.


I.7 Cancer over the long run
The charts below provide longer-run trends in cancer death rates, from 1930 in the United States, and lung cancer death rates across a number of countries since 1950.
Overall, particularly in lung cancer deaths, we see a significant rise, peak and then decline in cancer death rates. In the United States, this rate peaked in the 1980s in men (and not until the early 2000s for women). In the UK this peak was earlier in men (1970s), but similar in Italy (1980s). These trends are most tightly correlated to the increase, then reduction in smoking rates through governmental and health policies.


I.8 Cancer survival rates
Despite increasing global cancer deaths, cancer death rates across many types have been falling. This is partly attributed to earlier detection, and improved treatment: both of these factors have contributed to a significant increase in cancer survival rates across the world.
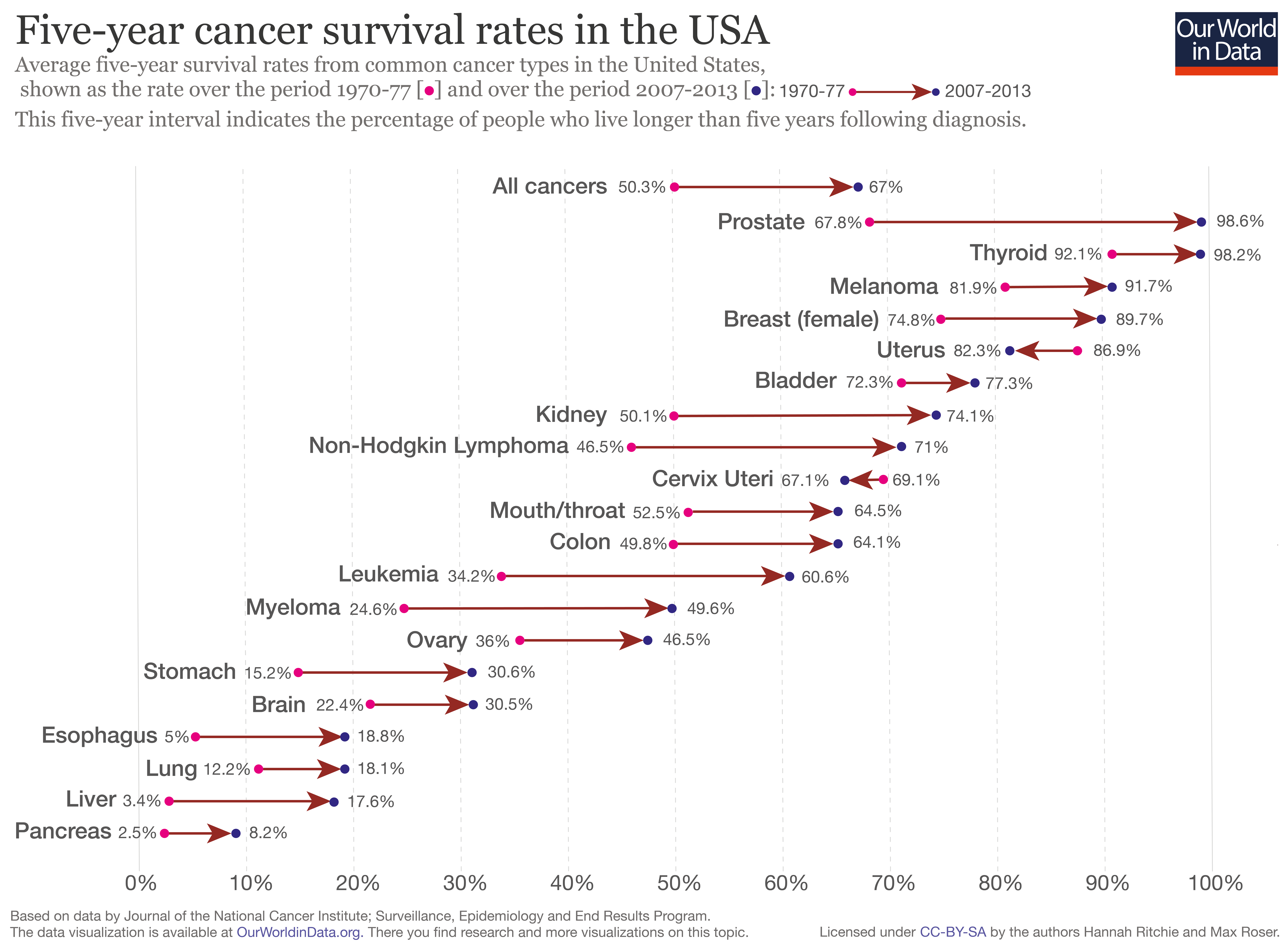
In the visual below we see the change in five-year survival rates (that is, the share of those diagnosed with cancer who survive at least five years following diagnosis) from the 1970s (1970-77) to 2007-2013 (this is the latest data available given the need for a five-year period). Overall we see that survival rates from all cancers have increased from 50 to 67 percent. This results from the combination of both early detection and improved treatment.
This change, however, varies significantly by cancer type. Progress in some has been very large: survival rates from prostate cancer, for example, have increased from 68 to almost 99 percent over this period. At the other end of the scale, five-year survival rates of uterus and cervix uteri cancers have actually declined since the 1970s. We still see major differences in survival rates overall: some, such as prostate and thyroid have a 98-99 percent five-year survival rate; those at the bottom of the spectrum (pancreas, liver, lung, & esophagus) have less than 20 percent probability.
The US National Cancer Institute also published data on five-year survival rates by sex and race. This data is available in the charts below. Overall we see similar trends, with prostate, thyroid, skin and breast cancer have the highest survival rates, and pancreas, liver, lung and esophagus the lowest. It is also the case that survival rates with black demographics (both for males and females) tend to be lower on average than that of white individuals.


Global data on cancer survival rates is typically much less readily available. In the charts below, we provide the widest coverage across countries of five-year survival rates by cancer type. This data is not available for all countries, however does cover a range of income levels. You can explore the range of countries using the "Change country" selection in the interactive chart below.

Also shown below are comparison of how five-year survival rates for lung, breast and liver cancer vary across the world. Here, we see wide variations; in lung cancer, Japan has the highest five-year survival rates at approximately 30 percent (in contrast to Chile, Bulgaria and Mongolia which has less than 7 percent). In breast cancer, higher income countries in particular across North America, Europe and Oceania tend to have five-year survival rates over 80 percent. This is almost double that of the lowest nation with available data - Jordan - at only 43 percent.



II. Correlates, Determinants & Consequences
II.1 Are cancers caused by genetic or external/risk factors?
Are cancers caused by genetic factors, or determined by external factors such as behavioural, lifestyle and environmental exposure? The relative contribution of genetic factors (DNA replication and tissue type) versus external exposure has been a dominant topic within cancer research. The outcomes of such studies are highly important — if genetic factors are found to be dominant then early detection and understanding of the relative vulnerability of different DNA and tissue variations arguably present the best opportunity to reduce cancer burden. In contrast, if external and environmental risk factors dominate, then lifestyle choice which reduces risk exposure is crucial for this reduction.
In a 2015 paper by Tomasetti & Vogalstein in Science, the authors conclude that only one-third of cancers are attributable to environmental factors or inherited predispositions; the vast majority result from “bad luck,” that is the random mutations which can occur when DNA replicates in normal non-cancerous cells.4 This study therefore argued that, beyond some cancer types which are deterministic (D-tumors) and can be reduced through lifestyle factors or vaccines, the most promising approach to reduction of cancer deaths across most cancers (replicative, R-tumors) is early detection.
This paper has been highly contest within the scientific literature. A number of later publications in Science provided a rebuttal to these conclusions, suggesting analytical flaws in the prior analysis, and epidemiological evidence which suggests otherwise.5,6,7 Such studies have argue that the role of 'chance' in cancer development was overstated by Tomasetti & Vogelstein, and the role of environmental exposures was understated. Wu et al. (2016) published in a study in Nature which concluded that intrinsic factors (which relates to the 'bad luck' DNA replication) account for less than 10-30 percent of cancer development, with the remaining (majority) share coming from extrinsic risk factors (which are external environmental exposures).8
The IHME, Global Burden of Disease (GBD) study attempt — using risk-exposure relationships — to provide attribution of certain risk factors to disease burden and mortality outcomes.9 These risk factors include a wide range, including smoking, diet and nutrition, obesity, alcohol intake, air pollution, & environmental exposures, such as carcinogens.
In the chart below we see IHME estimates of the share of global cancer deaths which are attributed to one of these major risk factors. For example, 84 percent of tracheal, bronchus and lung cancer deaths are attributed to risk factors such as smoking and air pollution. The remaining share of deaths we would therefore assume no attribution to risk factors, and would occur naturally in the absence of such risks (i.e. deaths from lung cancer which would result if no one smoked, zero air pollution etc.). Note that IHME risk factors do not account for sun exposure, which is a known risk factor for skin cancer. Attribution for skin cancers in the data below are therefore an underestimate.

II.2 Cancer by income, poverty and inequality level of the country
Cancer prevalence by income
The visualisation below shows the relationship between the prevalence of cancer (of any form) versus average income. Overall we tend to see lower prevalence of cancers at very low incomes, with a significant rise and positive correlation with income from around $9,000 PPP-adjusted income per year. Note that this does not compare the impact of income or poverty rates within individual countries, where associated lifestyle factors may have an impact on cancer prevalence.

Cancer deaths by income
Whilst cancer prevalence tends to show a positive relationship to income, death rates from cancer incorporate several factors: cancer prevalence, detection and treatment. When we compare cancer death rates across income, inequality and poverty rates (as shown in the charts below), there appears to be little relationship between countries. Note that this does not compare the impact of income or poverty rates within individual countries, where associated lifestyle factors may have an impact on cancer prevalence, early detection and treatment rates.



Cancer survival rates by income
Due to poorer data availability and standardisation of five-year cancer survival rates across the world, it is more difficult to determine any correlations across the full spectrum of incomes. However, in the charts below we show five-year survival rates (following diagnosis), versus GDP per capita for countries with such data available.
As we see, this relationship can vary significantly depending on cancer type. Five-year survival rates from breast cancer typically show a positive relationship: an increase in average income tends to be correlated to an increase in breast cancer survival rates. This is particularly true at lower-to-middle incomes, with a tailing off towards high incomes. The relationship in lung cancer survival rate is less well-established. There is significant variability in five-year survival rates between countries of a similar income.


III. Data Quality & Definition
In this entry we define cancer deaths in three fundamental ways:
- Absolute (total) number of cancer deaths;
- Cancer death rate: this reports the number of deaths per 100,000 individuals within a given population;
- Age-standardized death rate: this reports the number of deaths per 100,000 individuals assuming a constant and consistent age-structure of population between countries and across time.
These measures vary in the information they provide. Absolute (total) number of cancer deaths & prevalence figures provide an important indication of the total cancer burden within a given country or society. This is an important metric for a number of reasons, including the need for management and provision of adequate health services (which is dependent on the total societal burden, not just the incidence or risk for a given individual).
However, total number of cancer deaths fails to correct for population size and age. Cancer deaths can therefore rise as a result of higher cancer prevalence and/or poorer treatment, but also due to an increase in total population or an aging population. Cancer death rates correct for changes in population size, age-standardized death rates correct for population size and age structure. Age-standardization therefore gives a more indicative measure of the prevalence and incidence of underlying cancer risk factors between countries and with time without the influence of demographic and population structure changes.
IV. Data Sources
Institute of Health Metrics and Evaluation (IHME), Global Burden of Disease (GBD)
- Data: Death rates, absolute number of deaths and DALYS across all cancer types
- Geographical coverage:Global, across all regions and countries
- Time span:Most metrics available from 1990 onwards
- Available at: Online here
International Agency for Research on Cancer (IARC)/World Health Organization (WHO)
- Data: Cancer incidence and mortality of major types of cancer by sex
- Geographical coverage: Approx. 180 countries
- Time span: 1950-2002
- Available at: IARC and WHO's Globocan 2012 website, and at Gapminder.org
- On Gapminder, search for “cancer” in the search box to find the data files.
National Cancer Institute (NCI) Surveillance, Epidemiology, and End Results (SEER) Program
- Data: Cancer mortality and incidence for over 30 types of cancers by race/ethnicity, sex and age
- Geographical coverage: United States
- Time span: 1975-2010
- Available at: SEER Cancer Statistics Review website